PRP Knee Injection Vancouver
Platelet Rich Plasma PRP Knee Injection Vancouver
We offer ultrasound-guided PRP joint injections. We can also inject muscles, ligaments and tendons. PRP is a minimally invasive, non-surgical option that can alleviate pain, improve mobility and reduce inflammation resulting from injuries or chronic conditions. More and more patients are choosing PRP joint injections, especially for knee osteoarthritis, but it’s important to understand how it works and what to look for in a PRP provider.
Platelet Rich Plasma for muscle, tendon, ligament and joint injuries
PRP Injections may be a safe and effective, natural treatment for many types of musculoskeletal injuries and conditions. For instance, chronic tendon injuries like tennis elbow or jumper‘s knee can often take months to heal. Adding a PRP shot can help to speed up the healing process, reduce pain and allow you to get back to normal activity sooner.
PRP for Osteoarthritis
Osteoarthritis is a disease involving degeneration of articular cartilage, the smooth, white substance covering the ends of each bone, wears down. This can cause the bones to rub against each other, resulting in pain, swelling, and stiffness. People may develop osteoarthritis because of the normal aging process or as a result of previous injury. Genetics may also play a role.
Osteoarthritis is often treated with medications such as acetaminophen (Tylenol), ibuprofen (Motrin/Advil), physiotherapy, and other anti-inflammatory medication. When these are not enough, sometimes cortisone injections or hyaluronic acid is tried. However, this may not be a good idea as some studies have shown that cortisone may actually worsen joint destruction over time. On the other hand, MRI studies have shown no worsening of knee joints even up to 24 months after a single PRP session.
Unlike cortisone and other medication, PRP is a natural substance, derived from your own body which contains growth factors and cytokines which have been shown to promote tissue healing and regeneration. PRP therapy has been shown in many studies to be superior to cortisone and hyaluronic acid injections.
Sometimes the condition is so severe that no type of treatment will help. As a last resort, a joint replacement may be performed by an orthopedic surgeon.
How does Platelet-Rich Plasma work?
PRP, or platelet rich plasma, contains different growth factors that stimulate new hair growth and reduce hair loss. The treatment involves taking a sample of your blood, then processing these blood cells using a centrifuge to create a high concentration of platelets in plasma. Please see this post for what is PRP.
PRP is injected into the area of concern, such as a joint, tendon, or ligament. Platelets release growth factors which stimulate natural healing, collagen and tissue regeneration by recruiting stem cells to the damaged area and improved blood flow.
What are the Risks of PRP Joint Injections?
Overall, platelet rich plasma injections are very safe and well tolerated. Because PRP comes from a sample of your own blood, there is virtually no chance of allergic reaction.
PRP, like any other injection, has the following risks:
- Pain, bruising, infection,
- Decreased mobility, especially in the short term as the PRP creates more inflamation and swelling
PRP should only be prepared and given by a properly licenced and trained physician. For safety, make sure that the provider is using PRP kits that are approved by Health Canada (or the FDA in the USA).
Stem cells vs PRP for Joint Arthritis
It used to be thought that stem cells work better than PRP, but consider this:
A recent study compared stem cells (derived from fat) to PRP injections. The researchers found that PRP was just as effective as stem cells, except in severe arthritis. Interestingly, even in severe arthritis, stem cells only provided better relief of symptoms for the first 6 months. After that, it was equal. MRI imaging for both therapies showed no worsening of the arthritis for up to 2 years after a single injection of either PRP or stem cells.1 Similar results have been found using stem cells from bone marrow.
In other words, the benefits of PRP may be just as good as stem cells.
PRP vs Cortisone Injections: which is better?
Although Cortisone may offer better short term relief, it carries the risk of worsening arthritis over time. Refer to the following video about the risks of cortisone injections:
Who is a good candidate for PRP joint injections?
PRP may be an effective treatment option to stimulate healing in any injured area, including joints, tendons and ligaments. Mild to moderate arthritis responds best to PRP and has the most supporting evidence for improvement even after one treatment. However, when the extent of damaged tissue or knee pain is more severe, platelet-rich plasma therapy may not be the best treatment.
How many PRP injections will I need?
The number of injections may vary depending on the area being treated. For mild to moderate conditions, a single session may be enough. In other cases, the doctor may recommend multiple sessions (usually 4-6 weeks apart) as part of your treatment plan.
Who should NOT get PRP Joint Injections?
Certain conditions are contraindicated for having PRP Joint Injections, like active infection or very low platelet counts. In addition, PRP Joint Injections will simply not work as well for patients with more advanced arthritis as it works best for mild to moderate cases. PRP Joint Injections have not been studied as well for certain areas and conditions, such as the hip.
How much does PRP joint injection cost in Vancouver BC?
PRP joint injections range in price from $400 (naturopathic) to over $1500 CAD. In the USA cost ranges from $500 to $1500 USD. At our clinic, it starts from $600 for an ultrasound guided PRP injection. Consultation for joints is free, with no obligation.
What is the best type of PRP for joint injections?
Ideally, the best PRP for joint problems should have the following characteristics:
- Platelet concentration between 1-2 million per microliter.
- Platelet composition higher than 95% (low red blood cells)
- White blood cell concentration lower than baseline (less than 4,000 per µL)
- Count / Dose : the total dose of platelets should be 5-10 billion per treatment, approximately 4-6 mL at 1-2 million/µL per joint.
- The only way to be sure of the above characteristics is to use a hematology analyzer to check the PRP just before use.

Why choose PRP Medical Aesthetics?
We use only the highest concentration and purity PRP for all our joint injections. We have tested and compared our PRP to others and the results speak for themselves.

Steps of PRP injection therapy in at PRP Medical Aesthetics
There are several steps to having a PRP Joint Treatment at PRP Medical Aesthetics Clinic:
- Blood draw. We take about 50 – 100mL of blood. This is 2-4x the small amount of blood that most clinics take. This is necessary to have enough platelets in the starting sample.
- With sample, we test your baseline platelet counts using our hematology analyzer. If you have low platelets, we may recommend drawing more blood.
- We carefully proces your blood using a specialized centrifuge. This process usually takes about an hour as we have to go through several steps. A double-spin process is needed to obtain the highest possible concentration.
- We use a calibrated hematology analyzer to test the platelet concentration at several steps during this process.
- The final step to ensure quality: We test your sample for concentration, composition (purity), and calculate the final dose of platelets.
- Please note, if the final product is not concentrated enough, we may not perform the treatment as you will likely not see results. This hardly ever happens, but if it does, we can usually still get the procedure done, just not on the same day. We may need to do lab tests to determine if there is an underlying health problem, or sometimes start with more blood.
- Once everything is ready, the area is cleaned and numbed with a small amount of lidocaine.
- Dr. Yam will use an ultrasound machine to carefully inject the PRP into the proper area of the joint.
An example of PRP we prepared for an knee injection, with the hematology analysis report for it:
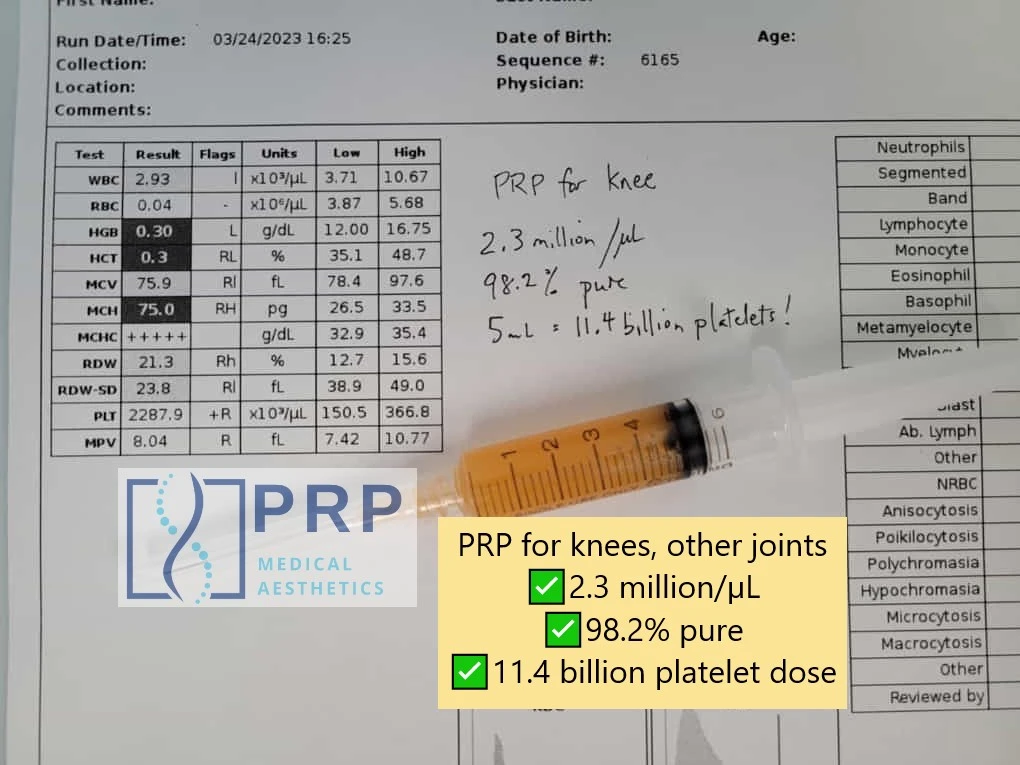
We would consider this an ideal sample of PRP to use in the joint, as the concentration is approximately 2.3 million platelets/µL, and it is 98.2% pure with only 1.7% RBC and 0.1% WBC. With 5 mL available, this is a dose of 11.4 billion platelets, which is enough for a proper treatment.
What does the Research Say about PRP Treatment for Arthritis?
Based on a rapidly growing body of evidence, more and more doctors, including sports medicine and orthopedic specialists, are starting to recommend PRP as the first choice for osteoarthritis of the knee. There is also evidence of benefit in other conditions, but it is not as robust.
Published reviews of PRP for knee osteoarthritis:
- A recent meta-analysis published in December 2021 in the medical journal Cartilage looked at 34 Randomized controlled trials (RCTs) comparing PRP joint injections with placebo or other injectable treatments and concluded that the PRP provides better results than other injectable options.2 The benefit appears to increase over time, being most apparent at 6-12 months after PRP joint injection treatment.
- A systematic review and meta-analysis study in the American Journal of Sports Medicine from January 2021 looked at PRP joint injections vs hyaluronic acid (HA) for knee osteoarthritis and showed that mean improvement was higher in the PRP group (44.7%) than the HA group (12.6%) for a standardized WOMAC score after almost 1 year follow-up.3
- A systematic review and meta-analysis from August 2021, also in the American Journal of Sports Medicine concluded that PRP Joint Injections showed improved outcomes when compared to other injectables, including cortisone, hyaluronic acid and placebo.4
- A systematic review and meta-analysis from the Journal of Orthopaedic Surgery and Research in 2017 looking at only randomized controlled trials also concluded that PRP joint injections are probably more effective in terms of pain relief and function improvement than other injections, including saline, hyaluronic acid, ozone, and cortisone.5
- A systematic review from the Journal Arthroscopy in 2016 looked at six studies involving 739 patients and concluded that in patients with symptomatic knee osteoarthritis, PRP joint injections are better than hyaluronic acid injections up to 12 months after treatment in terms of pain relief and function.6
Not all studies show benefit
Although many studies, systematic reviews and meta-analysis have been published on PRP Joint Injections, not all of them are as conclusive as the ones above. A recent updated systemic review of orthobiologics, which included PRP joint injections as well as various sources of stem cells, concluded that despite the growth of the technology, there was uncertain efficacy.7
A possible reason why PRP may not work in certain cases
Part of the reason for the uncertainty in the use and results of PRP Joint Injections, as well as other uses of PRP is the lack of standardization. Unfortunately, many of the PRP kits being used today do not provide high quality PRP and often this may not even be known by the clinics who are offering PRP joint injections. The only way to be certain of the quality and concentration of PRP being used is to test it directly, which is why we use a hematology analyzer at our clinic to check the quality and concentration of every PRP treatment given. For more information, see this post on quality and concentration.
Frequently Asked Questions
How many PRP joint treatments are needed?
The number of PRP treatments needed for arthritis, joint pain, sports injuries, etc will vary depending on several factors:
- Age and how long the condition has been present
- How severe the condition is (moderate arthritis will not respond as well as mild cases)
- Other underlying health conditions, e.g. diabetes
- Overall health and physical condition
What should be avoided before a PRP treatment?
In general, please avoid smoking, alcohol, and medications or supplements which may interfere with platelet function. These include anti-inflammatory medication (e.g. Advil, Motrin, Ibuprofen, Aleve, Naprosyn, etc) and some supplements like glucosamine chondroitin, Ginkgo Biloba, ginseng, garlic, green tea, ginger, Omega 3 fatty acids (fish oil), Vitamin E. Try to avoid these supplements for 5-7 days prior to your treatment.
What should you eat or drink before a PRP treatment?
In general, a healthy diet with lots of clear fluids is helpful before PRP treatments. Stay hydrated with lots of clear fluids. Avoid excess sugary drinks like juice or pop. Avoid alcohol. Fatty foods should be avoided for about 4 hours prior to PRP treatments. Ideally, do not to eat for 2 hours prior to treatment as this can make the plasma more lipemic.
Should I stop any medication before my PRP treatment?
No. Never stop any medication which has been recommended by your doctor or health care provider without consulting with them first. Stopping medication on your own could be lead to harmful effects on your health.
What to do after PRP Joint Injections?
After PRP Joint Injections, try to rest the treated area for the rest of the day. Avoid strenuous physical activity for at least five days following which you may gradually return to activity. Pay attention to your body and reduce the intensity if your symptoms are worsening. If possible, avoid anti-inflammatory medications after PRP Joint Injections as these may interfere with the effectiveness of the PRP.
When will I see results after PRP Joint Injections?
Typically, patients may see improvement starting around 2 weeks although some have reported improvement in much less time. Even if you are feeling better, remember not to push too hard at first to give your body time to recover. If you are working with the physiotherapist, be sure to let them know about your PRP Joint Injections.
Please see this page for instructions following PRP injections
Considering PRP? To Please feel free to schedule a free consultation with Dr. Yam today.
Academic References
- 1.Zaffagnini S, Andriolo L, Boffa A, et al. Microfragmented Adipose Tissue Versus Platelet-Rich Plasma for the Treatment of Knee Osteoarthritis: A Prospective Randomized Controlled Trial at 2-Year Follow-up. Am J Sports Med. Published online August 19, 2022:2881-2892. doi:10.1177/03635465221115821
- 2.Filardo G, Previtali D, Napoli F, Candrian C, Zaffagnini S, Grassi A. PRP Injections for the Treatment of Knee Osteoarthritis: A Meta-Analysis of Randomized Controlled Trials. CARTILAGE. Published online June 19, 2020:364S-375S. doi:10.1177/1947603520931170
- 3.Belk JW, Kraeutler MJ, Houck DA, Goodrich JA, Dragoo JL, McCarty EC. Platelet-Rich Plasma Versus Hyaluronic Acid for Knee Osteoarthritis: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Am J Sports Med. Published online April 17, 2020:249-260. doi:10.1177/0363546520909397
- 4.Singh H, Knapik DM, Polce EM, et al. Relative Efficacy of Intra-articular Injections in the Treatment of Knee Osteoarthritis: A Systematic Review and Network Meta-analysis. Am J Sports Med. Published online August 17, 2021:3140-3148. doi:10.1177/03635465211029659
- 5.Shen L, Yuan T, Chen S, Xie X, Zhang C. The temporal effect of platelet-rich plasma on pain and physical function in the treatment of knee osteoarthritis: systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. Published online January 23, 2017. doi:10.1186/s13018-017-0521-3
- 6.Meheux CJ, McCulloch PC, Lintner DM, Varner KE, Harris JD. Efficacy of Intra-articular Platelet-Rich Plasma Injections in Knee Osteoarthritis: A Systematic Review. Arthroscopy: The Journal of Arthroscopic & Related Surgery. Published online March 2016:495-505. doi:10.1016/j.arthro.2015.08.005
- 7.Delanois RE, Sax OC, Chen Z, Cohen JM, Callahan DM, Mont MA. Biologic Therapies for the Treatment of Knee Osteoarthritis: An Updated Systematic Review. The Journal of Arthroplasty. Published online December 2022:2480-2506. doi:10.1016/j.arth.2022.05.031
